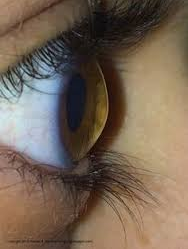
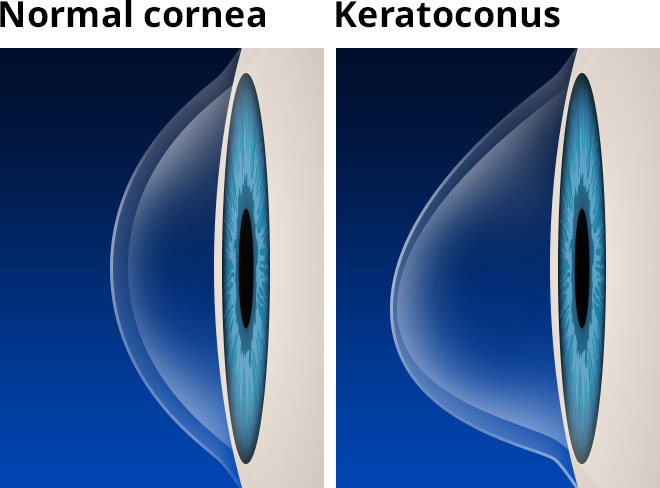
Your cornea is the clear, dome-shaped window at the front of your eye. It focuses light into your eye. Keratoconus is when the cornea thins out and bulges like a cone. Changing the shape of the cornea brings light rays out of focus. As a result, your vision is blurry and distorted, making daily tasks like reading or driving difficult.
What causes Keratoconus?
Keratoconus is a bilateral progressive disorder of unknown cause that typically starts during adolescence. It is usually an inherited corneal disorder which means that approximately 50% of family members may have it.
Symptoms of Keratoconus:
- Blurred and distorted vision
- Frequent changes in glass power or astigmatism (when your eye cannot focus as well as it should). As a result, you may need new eyeglass prescriptions often.
- Not being able to wear contact lenses. They may no longer fit properly and they are uncomfortable.
Diagnosis:
Your ophthalmologist will examine your cornea, and may measure its curve. This helps show if there is a change in its shape. Map your cornea’s surface using a special computer called as Corneal Topography is required to asses severity and management of Keratoconus. This detailed image shows the condition of the cornea’s surface.


Treatment:
In early stages of keratoconus, Rigid gas permeable (RGP) contact lenses can be tried. But in progressive cases, corneal collagen cross-linking is the treatment of choice.
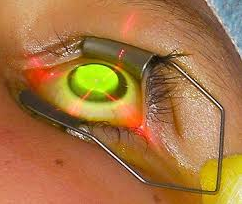
Collagen cross Linking with Riboflavin:
A new non-surgical, non-invasive treatment, based on collagen cross-linking with Ultraviolet A (UVA, 365nm) and riboflavin (Vitamin B 2), a photosensitizing agent is now available. This changes the intrinsic biomechanical properties of the cornea, increasing its mechanical strength. This increase in corneal strength has shown to arrest the progression of keratoconus.
However one needs to understand that Collagen cross-linking treatment is not a cure for keratoconus, rather, it aims to slow the progression of the condition. However, following the cross-linking treatment, it makes the patient more comfortable to wear contact lens. The main aim of this treatment is to arrest progression of keratoconus, and thereby prevent further deterioration in vision and the need for corneal transplantation.
Corneal transplant. When symptoms are severe, your ophthalmologist may suggest a corneal transplant.In this surgery all or part of diseased cornea is replaced with with healthy donor cornea tissue.
